Transform chronic pain management with evidence-based 2023 guidelines that prioritize personalized, multimodal approaches. Setting smart goals for chronic pain management alongside medical professionals creates a foundation for lasting relief. Recent research emphasizes integrating non-pharmaceutical interventions with traditional treatments, marking a significant shift in pain management protocols.
The updated 2023 guidelines reflect growing evidence supporting cognitive behavioral therapy, movement-based therapies, and mindfulness practices as essential components of comprehensive pain management. These evidence-based approaches, combined with careful medication management, offer new hope for the estimated 7.6 million Canadians living with chronic pain.
Medical professionals now recognize that successful pain management requires a balanced approach considering physical, emotional, and social factors. This holistic perspective, supported by recent clinical studies, provides better outcomes than single-modality treatments alone. The latest guidelines emphasize patient education, self-management strategies, and regular assessment of treatment effectiveness, ensuring that pain management plans evolve with patient needs.
What’s New in Pain Management for 2023
Evidence-Based Treatment Approaches
Recent research has highlighted several effective approaches for managing chronic pain, combining both pharmacological and non-pharmacological treatments. Physical therapy continues to show strong evidence for pain reduction, particularly when combined with targeted exercise programs. Studies indicate that graduated exercise therapy, starting with gentle movements and gradually increasing intensity, helps improve function and reduce pain levels.
Cognitive behavioral therapy (CBT) has emerged as a crucial component in pain management, with new research supporting its effectiveness in changing pain perception and developing better coping strategies. Mind-body techniques, including mindfulness meditation and breathing exercises, have also demonstrated significant benefits in pain reduction and improved quality of life.
Medical cannabis has gained more recognition as a treatment option, particularly for specific types of chronic pain, though its use should be carefully monitored by healthcare providers. Additionally, innovative approaches like pain neuroscience education and acceptance and commitment therapy (ACT) are showing promising results in helping patients understand and manage their pain more effectively.
Interdisciplinary treatment programs, which combine multiple evidence-based approaches under one coordinated plan, continue to demonstrate the best outcomes for chronic pain management.
Moving Away from Opioid-Centric Care
Recent guidelines emphasize a significant shift away from opioids as the primary treatment for chronic pain. Healthcare providers now focus on multimodal approaches that combine various non-opioid treatments. These include physical therapy, cognitive behavioral therapy, and alternative medicine practices like acupuncture and mindfulness meditation.
Exercise programs, particularly those tailored to individual capabilities, have shown remarkable success in managing chronic pain. Many patients find relief through low-impact activities such as swimming, yoga, or guided stretching routines. Additionally, emerging research supports the use of CBD for pain management as part of a comprehensive treatment plan.
Non-opioid medications, such as anti-inflammatory drugs, nerve pain medications, and topical treatments, are increasingly recommended as first-line options. This approach helps reduce the risk of dependency while still providing effective pain relief. Healthcare providers also emphasize the importance of lifestyle modifications, including stress management, proper sleep hygiene, and dietary adjustments, which can significantly impact pain levels and overall quality of life.
Integrated Treatment Strategies
Physical Therapy and Exercise
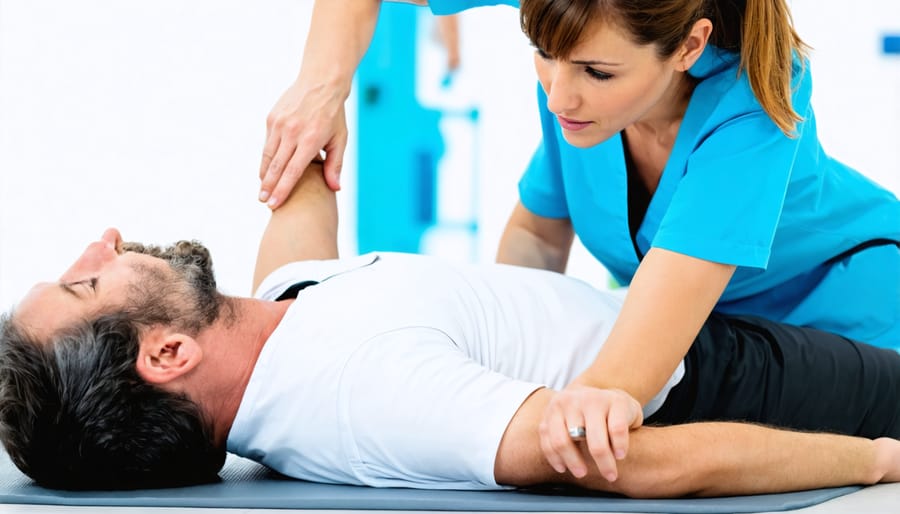
Physical activity remains a cornerstone of chronic pain management, with updated guidelines emphasizing the importance of individualized exercise programs. Before starting any exercise routine, consult with healthcare providers to ensure it’s appropriate for your underlying medical conditions.
The latest recommendations advocate for a gradual approach to movement therapy, starting with gentle exercises and progressively increasing intensity. Low-impact activities such as walking, swimming, and stationary cycling are particularly beneficial for those new to exercise. Aim for 150 minutes of moderate physical activity per week, divided into manageable sessions of 10-30 minutes.
Supervised physical therapy programs have shown enhanced effectiveness when combined with home exercises. Focus areas include:
– Stretching and flexibility exercises
– Strength training with emphasis on core stability
– Balance and coordination activities
– Gentle aerobic exercises
– Mind-body practices like tai chi and yoga
The 2023 guidelines strongly support the integration of movement tracking through smartphones or fitness devices to monitor progress and maintain motivation. Regular movement breaks throughout the day are also recommended to prevent pain flare-ups, especially for those with sedentary lifestyles.
Remember that some initial discomfort is normal when starting an exercise program, but pain should not significantly worsen during or after activity. Listen to your body and adjust your routine accordingly.
Mental Health Support
The psychological impact of chronic pain can be significant, making mental health support a crucial component of comprehensive pain management. Research shows that individuals experiencing chronic pain are more likely to develop anxiety and depression, which can, in turn, intensify pain perception and create a challenging cycle.
Cognitive Behavioral Therapy (CBT) has emerged as a leading psychological intervention for chronic pain management. This approach helps individuals identify and modify negative thought patterns and behaviors related to their pain experience. Through CBT, patients learn valuable coping strategies, stress management techniques, and pain acceptance methods that can significantly improve their quality of life.
Mindfulness-based interventions have also shown promising results in pain management. Regular mindfulness practice can help reduce pain-related stress and anxiety while improving overall emotional well-being. Techniques such as guided imagery, deep breathing exercises, and meditation can provide effective tools for managing pain-related distress.
Support groups and peer counseling offer additional benefits by connecting individuals with others who share similar experiences. These connections can reduce feelings of isolation and provide practical coping strategies through shared experiences.
Healthcare providers now recognize that addressing mental health is not just an optional add-on but an essential component of effective pain management. Many pain clinics offer integrated care that combines physical treatments with psychological support, ensuring a holistic approach to pain management.
Lifestyle Modifications That Make a Difference
Nutrition and Anti-Inflammatory Foods
Diet plays a crucial role in managing chronic pain, with certain foods having natural anti-inflammatory properties that can help reduce pain and discomfort. Research shows that a Mediterranean-style diet, rich in whole foods and plant-based ingredients, can significantly impact pain levels and overall inflammation in the body.
Key anti-inflammatory foods to include in your diet are fatty fish (such as salmon and mackerel), which contain omega-3 fatty acids, and colorful fruits and vegetables high in antioxidants. Berries, leafy greens, and cruciferous vegetables like broccoli and cauliflower are particularly beneficial. Include herbs and spices such as turmeric, ginger, and cinnamon, which have proven anti-inflammatory properties.
Equally important is avoiding foods that can increase inflammation. Limit processed foods, refined sugars, and excessive red meat consumption. Studies indicate that reducing these inflammatory triggers can lead to noticeable improvements in pain levels within several weeks.
Consider these practical dietary changes:
– Start your day with anti-inflammatory smoothies
– Include at least one serving of fatty fish weekly
– Add turmeric to soups and stews
– Snack on nuts and seeds rich in healthy fats
– Choose whole grains over refined carbohydrates
Remember to stay well-hydrated, as proper hydration helps maintain joint function and reduces inflammation. While dietary changes alone may not eliminate chronic pain, they can be an effective part of a comprehensive pain management strategy.

Sleep and Stress Management
The impact of sleep quality and stress levels on chronic pain cannot be overstated. Research shows that poor sleep can intensify pain sensations and create a challenging cycle where pain disrupts sleep, and lack of sleep worsens pain. To break this cycle, experts recommend maintaining consistent sleep schedules and creating a relaxing bedtime routine.
Stress management is equally crucial in pain management. When we’re stressed, our bodies produce hormones that can increase inflammation and muscle tension, potentially amplifying pain signals. Incorporating stress-reduction techniques into daily life can help manage both stress and pain levels effectively.
Consider these evidence-based strategies:
– Practice relaxation techniques like deep breathing or progressive muscle relaxation
– Maintain good sleep hygiene by keeping your bedroom cool, dark, and quiet
– Set a regular bedtime and wake-up time
– Limit screen time before bed
– Try mindfulness meditation or gentle yoga before sleep
– Use stress-management apps or guided relaxation recordings
Working with healthcare providers to address sleep issues and stress is essential for developing an effective pain management plan. They may recommend cognitive behavioral therapy for insomnia (CBT-I) or other specialized interventions to improve sleep quality and reduce stress-related pain amplification.
Technology and Pain Management
Digital Health Tools
Modern digital health tools have revolutionized how we track and manage chronic pain. Pain management apps like Manage My Pain and PainScale help users log their pain levels, triggers, and medication schedules. These apps create detailed reports that can be shared with healthcare providers, leading to more informed treatment decisions.
Wearable devices equipped with biometric sensors can monitor physical activity, sleep patterns, and stress levels – all factors that influence pain intensity. Some advanced devices offer features like guided breathing exercises and medication reminders to help users stay on track with their pain management routines.
Virtual reality (VR) technology has emerged as a promising tool for pain relief, with studies showing its effectiveness in reducing pain perception through immersive distraction techniques. Several Canadian healthcare facilities now offer VR therapy as part of their pain management programs.
Mobile meditation and mindfulness apps can help develop stress-management skills, while specialized pain education platforms provide evidence-based information and coping strategies. These digital solutions work best when integrated into a comprehensive pain management plan developed with healthcare providers.

Emerging Treatment Technologies
In 2023, several innovative treatment technologies are showing promise in chronic pain management. Virtual reality (VR) therapy has emerged as an effective tool, helping patients manage pain through immersive distraction and guided relaxation exercises. Research shows that VR can reduce pain intensity by up to 40% during sessions.
Neurostimulation devices have also advanced significantly, with new portable options allowing patients to manage pain at home. These devices use electrical impulses to interrupt pain signals and can be controlled through smartphone apps, giving patients greater control over their treatment.
Artificial intelligence-powered pain management systems are now being used to track patterns and suggest personalized interventions. These systems analyze factors like activity levels, sleep quality, and pain triggers to provide tailored recommendations.
Additionally, regenerative medicine treatments, including platelet-rich plasma (PRP) therapy and stem cell treatments, are becoming more refined and accessible. While still being studied, early results suggest these treatments may help repair damaged tissue and reduce chronic pain in some patients.
These emerging technologies complement traditional pain management approaches, offering new hope for those seeking relief from chronic pain.
Managing chronic pain effectively requires a comprehensive, personalized approach that combines various treatment strategies. The 2023 guidelines emphasize the importance of active patient participation and highlight several key principles for successful pain management. These include starting with non-pharmacological approaches, carefully considering medication options, and maintaining regular communication with healthcare providers.
Remember that everyone’s pain experience is unique, and what works for one person may not work for another. It’s essential to work closely with your healthcare team to develop and adjust your pain management plan as needed. The latest guidelines encourage a balanced approach that addresses both physical and emotional aspects of chronic pain.
Take proactive steps in your pain management journey by keeping detailed records of your symptoms, treatments, and their effectiveness. Don’t hesitate to discuss new treatment options with your healthcare provider, especially if your current plan isn’t providing adequate relief. Stay informed about emerging research and treatment options, but always verify new information with qualified healthcare professionals.
Most importantly, maintain hope and persistence in your pain management journey. While chronic pain can be challenging, the expanding range of treatment options and growing understanding of pain management offer increasing opportunities for improved quality of life. Reach out to support groups and healthcare providers to ensure you’re not facing this challenge alone.

